Testicular Cancer: Understanding, Detecting, and Treating One of the Most Curable Male Cancers Today
Testicular cancer is one of the most treatable forms of cancer, especially when detected early. As awareness continues to grow and medical research advances, men are gaining access to more effective screening, diagnosis, and treatment options. This detailed article explores what men need to know about testicular cancer, including causes, risk factors, treatment innovations, and long-term recovery considerations.

The Growing Importance of Awareness About Testicular Cancer
Testicular cancer primarily affects younger men, typically between ages 15 and 45. Despite its prevalence in younger age groups, early detection dramatically increases survival rates. Better public education and routine self-examinations are helping more men identify abnormalities sooner, improving treatment outcomes. Because testicular cancer progresses quickly, awareness is one of the strongest tools for saving lives.
Another reason awareness matters is that many symptoms can be subtle, easily ignored, or mistaken for minor issues such as muscle strain or infection. This makes education essential, particularly for men at higher risk. Public health campaigns now emphasize body awareness and regular self-checks as preventive steps.
In recent years, digital health platforms and online medical communities have further helped normalize discussions about testicular cancer, breaking down stigma and encouraging early medical consultation.
Understanding What Testicular Cancer Is
Testicular cancer begins in the testicles and typically forms in germ cells, which are responsible for producing sperm. Most cases fall into two main types: seminomas and non-seminomas. Seminomas grow slowly and respond very well to radiation and chemotherapy, while non-seminomas tend to grow faster but remain highly treatable.
Understanding the nature of the disease is essential because treatment varies depending on the cancer type and stage. Doctors use ultrasound imaging, blood tumor marker tests, and physical examinations to determine the presence and progression of testicular cancer.
Early-stage testicular cancer is almost always localized, making it easier to treat. Advanced stages may involve spread to lymph nodes or organs, but even then, cure rates remain high.
Key Risk Factors Associated With Testicular Cancer
Several risk factors increase the likelihood of developing testicular cancer. The strongest known risk factor is undescended testicles (cryptorchidism), where one or both testicles fail to move into the scrotum during infancy. Even after surgical correction, risk remains elevated.
Family history also plays a role. Men with fathers or brothers who developed testicular cancer face a higher risk. Additional factors include previous testicular abnormalities, infertility issues, and certain genetic conditions.
Though risk factors increase probability, many men diagnosed with testicular cancer have no known risks at all. This reinforces the importance of regular screening and self-awareness regardless of background.
Recognizing the Early Symptoms of Testicular Cancer
Early symptoms are often subtle, which makes self-examination crucial. The most common symptom is a painless lump in the testicle. Some men may notice swelling, heaviness, or discomfort, while others report a dull ache in the lower abdomen or groin.
In some cases, hormonal changes caused by testicular cancer can lead to breast tenderness or enlargement. These changes occur because certain tumors produce hormones that disrupt normal bodily functions.
Advanced symptoms may include back pain or shortness of breath if the cancer spreads. However, early detection remains far more common thanks to increased awareness and modern medical evaluations.
Evolution of Testicular Cancer Diagnosis
Diagnostic procedures have evolved significantly in recent decades. Today’s screening process typically begins with a physical exam, followed by an ultrasound—an imaging method that provides detailed views of the testicle’s structure.
Blood tests also play a key role. Tumor markers such as AFP, hCG, and LDH help doctors identify the type of testicular cancer and measure treatment response. These markers offer critical information even before surgery or radiation begins.
In complex cases, CT scans are used to determine whether cancer has spread. Because accuracy is vital to treatment success, diagnostic tools continue improving through research and technology development.
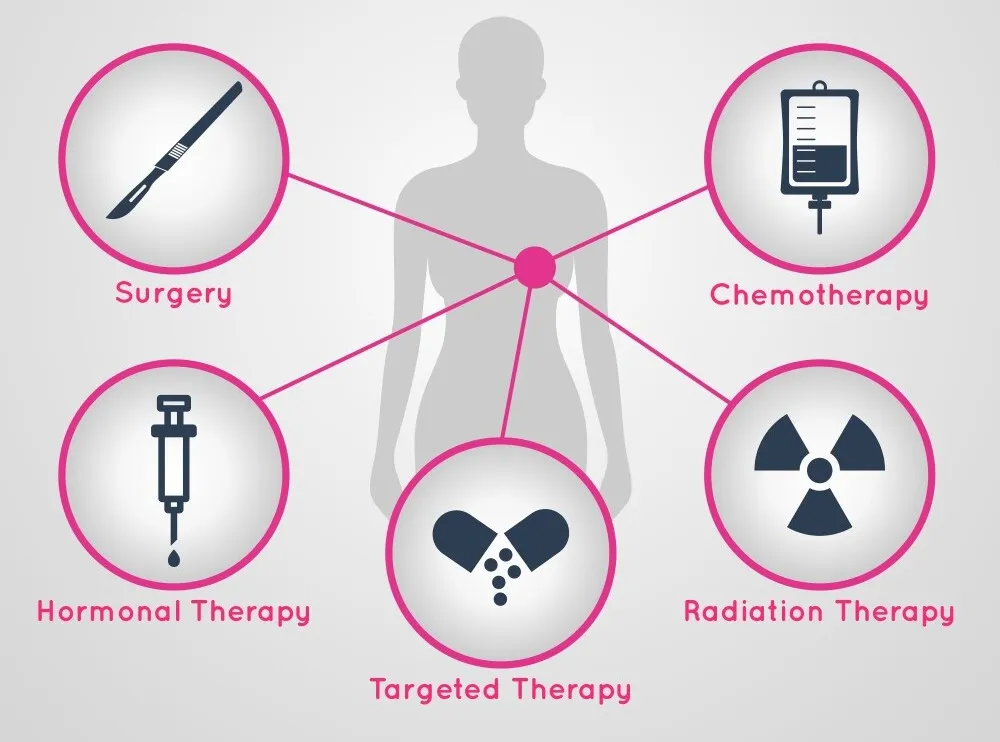
Standard Treatments for Testicular Cancer
Surgery, known as radical inguinal orchiectomy, is the first-line treatment in almost all cases. During this procedure, the affected testicle is removed, preventing further spread of cancer cells.
Depending on the cancer type and stage, additional treatments may include chemotherapy or radiation. Seminomas respond especially well to radiation, while non-seminomas typically require multi-drug chemotherapy regimens.
Many patients achieve complete remission with these treatments. Because testicular cancer has one of the highest survival rates among all cancers, early treatment offers excellent long-term outcomes.
Advances in Chemotherapy and Radiation Therapy
Modern chemotherapy drugs are more effective and less toxic than earlier formulas, significantly improving quality of life during treatment. Combination drug therapies can target fast-growing non-seminomas with high precision, increasing cure rates even in advanced cases.
Radiation therapy has also evolved. Specialists now use targeted beams to minimize exposure to healthy tissue, reducing long-term side effects. The ability to pinpoint cancer cells precisely has made radiation a cornerstone treatment for seminoma cases.
Continued advancements in both areas ensure that testicular cancer patients have access to safe, reliable treatment options that promote long-term health.
Fertility Preservation and Life After Treatment
Because testicular cancer affects reproductive organs, fertility is an important concern. Before treatment, many patients choose sperm banking, which offers long-term security for future family planning. Oncologists routinely discuss fertility preservation during initial consultations.
After treatment, most men return to normal sexual and reproductive health. However, regular monitoring is essential. Follow-up appointments typically include imaging tests, blood work, and physical exams to ensure cancer does not return.
Long-term survival rates are extremely high, giving survivors the opportunity to lead full, healthy, and active lives beyond testicular cancer.
Lifestyle Adjustments and Recovery After Testicular Cancer
Recovery involves both physical and emotional adjustments. Many men benefit from exercise, stress management, and nutrition planning as they regain strength. Support groups also play a vital role, offering encouragement from other survivors.
Mental health is equally important. Anxiety about recurrence is common, but counseling and medical reassurance help men maintain a positive outlook. Many survivors use their experience to promote awareness for early detection.
Over time, men adapt fully to life after testicular cancer, often becoming advocates for men’s health.
Future Research and Hope for Continued Advances
Research efforts continue to deepen our understanding of testicular cancer. Scientists are exploring genetic markers, targeted therapies, and new surgical strategies to further reduce recurrence rates.
Immunotherapy—already successful in other cancers—is showing promise as a future treatment option. Clinical trials continue to expand, offering more personalized therapies for patients worldwide.
The rapid pace of research ensures that testicular cancer survival rates will remain high and that treatments will become even less invasive in the years ahead.
Conclusion
Testicular cancer is one of the most treatable cancers today, offering excellent survival outcomes when diagnosed early. Understanding symptoms, staying aware of personal risks, and seeking timely medical care are critical steps for men’s health. Advancements in surgery, chemotherapy, and long-term recovery support make treatment safer and more effective than ever before. With ongoing research and growing awareness, individuals diagnosed with testicular cancer can look toward a future filled with hope, strength, and renewed health.